January 11, 2010 - By Sara Wykes

A pneumatic tube system at Stanford Hospital, run by chief engineer Leander Robinson, has some four miles of pipes.
Every day, 7,000 times a day, Stanford Hospital staff turn to pneumatic tubes, cutting-edge technology in the 19th century, for a transport network that the Internet and all the latest Silicon Valley wizardry can’t match: A tubular system to transport a lab sample across the medical center in the blink of an eye.
In four miles of tubing laced behind walls from basement to rooftop, the pneumatic tube system shuttles foot-long containers carrying everything from blood to medication. In a hospital the size of Stanford, where a quarter-mile’s distance might separate a tissue specimen from its destination lab, making good time means better medicine.
“Approximately 70 percent of the information on a patient’s chart is lab data,” said David Myrick, quality coordinator for the hospital’s clinical labs. “We conduct about 8 million tests a year, serving thousands of patients. We are going full blast, 24-7, at the highest level of testing. The tube system is part of a complex chain of events that ultimately give doctors the essential lab results they need to make decisions about our patients.”
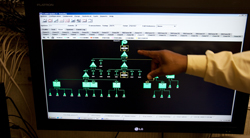
Hospital staff use computer montiors to punch in where they want to send a particular cylinder and then can follow a tiny icon that shows the package as it moves through the tubes. A special software system allows engineers to monitor the ebb and flow of traffic on the network.
The value of these pneumatic tube networks is not unique to Stanford—they are in use at hospitals nationwide—but SHC’s system, which also serves the adjacent Lucile Packard Children’s Hospital, is one of the largest in the country. Its architecture is a sophisticated design of switching points, waiting areas, sending and receiving points. It hosts 124 stations (every nursing unit has its own); 141 transfer units, 99 inter-zone connectors and 29 blowers. To help alert employees to the arrival of containers, the system has more than three dozen different combinations of chiming tones.
Such pneumatic tube systems date back to the early 19th century, when they drove the workings of postal services, department stores and other commercial businesses whose physical size demanded something faster than standard human pace. But those versions were usually designed to move paper. As computers and then the Internet made it possible to deliver data electronically without paper, tube systems lost their value for many industries.
But the technology endures—and thrives—in hospitals, thanks in part to more recent improvements in the delivery system. Originally, the tubes would arrive with a thud, a hard landing that could damage sensitive lab samples. Then in the late 1980s engineers figured out a way to control airflow to slow down the containers for a soft landing at their destination station.

Although tubes converge at key points, no cylinder has ever gotten stuck in the system.
At Stanford Hospital, before 1993, a team of about 20 people had the job of transporting the multitudes of tissue, medications and documents. However, the increasing size of the hospital, and the addition of two adjacent buildings—the Blake Wilbur Outpatient Clinic, the Stanford Cancer Center and Packard Children’s Hospital—made the tube system option the most modern solution. “We like the human touch,” said chief of staff Bryan Bohman, MD, “but we don’t like the human foot speed.”
Depending on the diameter of a tube, cylinders can reach speeds of up to 25 feet per second, about 18 miles per hour, far faster than any human could ever manage.
It was also a question of best use of employee time, if, as often happened, a courier wasn’t available when a specimen needed to get to the lab. Having a nurse leave a patient’s bedside for a minutes-long run to the lab made no sense.
Reliable speed is crucial when the system carries blood products, some of which are temperature-sensitive and, by regulations, must be discarded if not properly maintained. The tube system, said Gay Routh, lab operation services manager “is vital, very vital. I don’t know what we’d do without the tube system, especially when it comes to tests like those that happen in surgery. When arterial blood gases are sent from the operating room, we need to return results in a very short period of time, so physicians know if they need to change settings on a monitor. Years ago, before the tubes, we would get a phone call and we’d have to send somebody. It definitely slowed our turnaround time.”

Each cylinder can be used to transport tissue specimens, medications or blood products. They travel at a speed of roughly 18 miles per hour, which is far faster than a human messenger could move through the medical center.
Leander Robinson, the hospital’s chief engineer, commands the system from a small basement office, where computer monitors light up every time someone puts a container in a chute, types in a numerical address and presses the "send" button. The screen displays a tiny icon that reflects the container’s travel through various switches and transfers, but it moves so quickly it’s actually hard to track its passage. Even during the heaviest flow through the system, between noon and 2 p.m., a container can cover the longest start-to-finish distance—1,500 feet—in less than three minutes.
The system has a complete set of checks and balances, sensing where containers are needed and sending them. Some departments, such as the operating rooms, have dedicated lines that guarantee them a straight shot to the lab. “Blood products get first priority,” said Lee Chua, blood transfusion services manager.
The system does occasionally falter, but it’s operative 98.8 percent of the time, Robinson said. And no cylinder has ever gotten stuck in a tube, he said.
Robinson has software that monitors the system, charting its use station by station and watching especially those times when someone sends a cylinder “stat”—the highest priority coding.
It’s also a work in constant progress; the hospital continues to evolve and locations can change.
“The tube is everywhere,” Robinson said, “and the directories ever changing.”
The system “is amazing,” said Pam Ponti, assistant patient care manager, who sends and receives cylinders that affect surgical care. “I don’t know exactly how it knows where to go, I’m just happy that it does.”
Sara Wykes is a writer in the Stanford Hospital & Clinics communications office.
About Stanford Medicine
Stanford Medicine is an integrated academic health system comprising the Stanford School of Medicine and adult and pediatric health care delivery systems. Together, they harness the full potential of biomedicine through collaborative research, education and clinical care for patients. For more information, please visit med.stanford.edu.