December 8, 2009 - By Erin Digitale
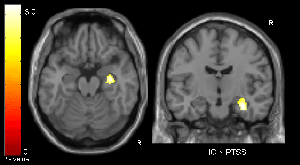
The bright regions in these scans (at left, a top-down view of the brain; at right, a view of the brain from the back of the head) indicate greater hippocampus activity in healthy children during memory recall than in children with PTSD symptoms.
Psychological trauma leaves a trail of damage in a child's brain, say scientists at the Stanford University School of Medicine and Lucile Packard Children's Hospital. Their new study gives the first direct evidence that children with symptoms of post-traumatic stress suffer poor function of the hippocampus, a brain structure that stores and retrieves memories. The research helps explain why traumatized children behave as they do and could improve treatments for these kids.
"The brain doesn't divide between biology and psychology," said Packard Children's child psychiatrist Victor Carrion, MD, the primary author of the new research. "We can use the knowledge we get from understanding brain function to improve the psychology of the individual and vice versa."
Extreme stressors such as experiencing abuse or witnessing violence can make children isolate themselves from family and friends, feel disconnected from reality, experience intrusive thoughts about the trauma and struggle in school. "Post-traumatic stress is not only about the traumatic memories; it really affects daily living," said Carrion, who is an associate professor of child and adolescent psychiatry at the School of Medicine and director of Stanford’s early life stress research program. The research was published online Dec. 8 in the Journal of Pediatric Psychology. (The paper's Digital Object Identifier, or DOI, is 10.1093/jpepsy/jsp112.)
The findings could be an important step toward better monitoring of PTSD treatments, which include psychotherapy techniques such as teaching relaxation exercises, helping children to construct a cohesive story about the traumatic event and helping them learn to cope with reminders of the trauma. Right now, psychologists assess such treatments by looking for improvements in symptoms, but that's a problem because the symptoms can fluctuate from day to day. "That method has the disadvantage that we don't know what's happening at the neural level," Carrion said.

Victor Carrion
To observe how kids' brains work after trauma, Carrion's team used functional magnetic resonance imaging to compare 16 young people who had PTSD symptoms with a control group of 11 normal youths. The scientists scanned the brains of the 10- to 17-year-old subjects during a simple test of verbal memory. Subjects read a list of words, then saw a similar list with new words added, and were asked which terms were present on the original list.
The hippocampus worked equally well in stressed and control subjects when the word list was first introduced. However, subjects with PTSD symptoms made more errors on the recall part of the test and showed less hippocampus activity than control subjects doing the same task.
Subjects with the worst hippocampus function were also most likely to experience a specific set of PTSD symptoms: Such impairment of the hippocampus was strongly correlated with "avoidance and numbing" symptoms of PTSD, including difficulty remembering the trauma, feeling cut off from others and lack of emotion.
Parents and other caregivers may find the new discoveries useful as they tend to traumatized children, Carrion said, particularly when children respond to trauma by withdrawing from people who are trying to help. Parents may sometimes misinterpret this behavior as a child's attempt to retaliate, when it actually represents an overload of the brain's normal mechanism for handling fear. "When parents understand that PTSD is real, they don't take it as personally," he said. "They become more available to their kids. That's good because the kids need them."
In the future, physicians and scientists may be able to use fMRI scans of the hippocampus to identify children who are at high risk of PTSD after mass catastrophes, added Carrion, who has consulted on response teams for natural disasters such as Hurricane Katrina and the February 2009 wildfires in southeastern Australia. However, larger studies of brain activity in pediatric PTSD are still needed to give a more detailed understanding of the disorder.
It's already clear that untreated PTSD can interfere with a child's normal brain development and increase the risk of other psychiatric conditions such as depression and substance abuse, Carrion concluded. "Early intervention is critical for children with post-traumatic stress," he said.
Carrion's team at Stanford included postdoctoral fellow Brian Haas, PhD; research associate Amy Garrett, PhD; child psychiatry fellow Suzan Song, MD; and Allan Reiss, MD, the Howard C. Robbins Professor of Psychiatry and Behavioral Sciences and professor of padiology and child psychiatrist at Packard Children's. The research was funded by grants from the National Institute of Mental Health; NARSAD, previously known as the National Alliance for Research on Schizophrenia and Depression; the American Foundation for Suicide Prevention; and the Aloha Foundation.
About Stanford Medicine
Stanford Medicine is an integrated academic health system comprising the Stanford School of Medicine and adult and pediatric health care delivery systems. Together, they harness the full potential of biomedicine through collaborative research, education and clinical care for patients. For more information, please visit med.stanford.edu.