August 7, 2009 - By Krista Conger

For the past eight years, scientists who wanted to use federal funds for research on human embryonic stem cells had to restrict their studies to 21 cell lines approved by the National Institutes of Health. But an analysis by a researcher at the Stanford University School of Medicine suggests that only two of those lines have been used routinely.
“I was surprised by these results,” said Christopher Scott, director of Stanford’s Program on Stem Cells in Society. “I never imagined that we would find that three-fourths of the requests would be for the same two cell lines.”
On the one hand, the findings raise concerns about the reauthorization process of cell lines under way at the NIH — if these lines are now excluded from federal funding due to ethical considerations, researchers may abandon them, and their previous research, in favor of other lines. On the other, the findings draw attention to the possibility that these two lines may have abnormalities or characteristics that make them not as useful as newer lines.
“Not only are scientists asking for these lines, they are publishing on them,” said Scott, a senior research scholar at Stanford’s Center for Biomedical Ethics. “They have become the reference standards against which new embryonic and iPS cell lines are being compared.” (An iPS cell is an adult cell that has been induced to look and act like a human embryonic stem cell; comparing them with existing embryonic stem cell lines is important, as there is much debate about whether these iPS cells are functionally equivalent to human embryonic stem cells.)
Scott collaborated with researchers from the Mayo Clinic and the University of Michigan to conduct the research, published Aug. 7 in Nature Biotechnology. Together they analyzed the number and timing of requests placed by scientists for human embryonic stem cell lines housed at the two largest stem cell banks in the country: the National Stem Cell Bank at the WiCell Research Institute in Madison, Wisc., and the Harvard Stem Cell Institute in Massachusetts.
Although the National Stem Cell Bank is meant to be the source of all NIH-approved lines, Scott and his colleagues found that at no time have all 21 lines been available for distribution; a maximum of 18 lines were available at the beginning of this year. Two cell lines, known as H1 and H9, made up the majority of requests — 941 out of 1,217, or 77 percent, since 1999. One other line, H7, was requested 111 times. In contrast, 13 of the previously approved lines were requested fewer than 10 times in the past decade.
Research on the three most-requested lines from the NSCB is prevalent in the scientific literature: 83 percent of 534 peer-reviewed publications from 1999 to 2008 discussed research on H9, 61 percent on H1 and 24 percent used H7 (the numbers exceed 100 percent because many studies used more than one cell line). In contrast, fewer than 36 percent of the publications used any of the other NSCB-curated cell lines.
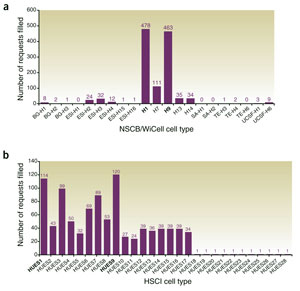
Two stem cell lines (top) comprise 77 percent of requests to the National Stem Cell Bank in this decade. About 25 percent of requests to the Harvard Stem Cell Institute (above) are for two other lines.
Requests for cell lines from the Harvard Stem Cell Institute included a wider selection of lines, but even these were still relatively narrow, the researchers found. The majority of these cell lines were created by Harvard researcher Douglas Melton with private funds. Of the 17 cell lines available since 2004, 234 of 946 requests, or 25 percent, were for one of two lines: HUES1 and HUES9.
Even though the Harvard stem cell lines increase the diversity available to researchers, their impact in the published research has so far been minimal: Only about 3 percent of the peer-reviewed articles included in Scott’s study reported research on the two most popular Harvard lines.
“It could be a first-mover advantage,” said Scott of the researchers’ bias toward just a few lines. “If one group publishes on a particular line, other groups want to replicate and extend that research.” It’s also possible, the authors theorize, that the complex thicket of federal and state restrictions on embryonic stem cell research simply made researchers skittish about branching off into new cell lines.
“The trick will be to avoid this kind of situation with the NIH’s new stem cell registry,” said Scott, referring to the system that the agency will be establishing to ensure that only research on approved lines gets federal funding. Future policies should be designed, he said, to preserve researchers’ ability to continue to work on these well-characterized lines while also encouraging them to plumb the new lines that are expected to become eligible for federal funding under the new regulations. “We’re starting with a very scarce resource, and we have to figure out how to make it high quality.”
The research was supported by the Stanford Institute for Neuro-Innovation and Translational Neurosciences, the National Science Foundation and the National Institutes of Health.
About Stanford Medicine
Stanford Medicine is an integrated academic health system comprising the Stanford School of Medicine and adult and pediatric health care delivery systems. Together, they harness the full potential of biomedicine through collaborative research, education and clinical care for patients. For more information, please visit med.stanford.edu.